Articolo del 07/05/2026
When patients receive their blood test results, the first figure they often check is their cholesterol. If the value is highlighted in red, alarm bells ring immediately. However, cholesterol is not a monolith, nor should it be interpreted as an isolated figure.
Understanding the distinction between HDL and LDL is vital. Even more critical is recognizing why these results must be evaluated by an Internal Medicine specialist before pursuing further diagnostic tests.
HDL vs. LDL: What Do They Truly Represent?
We discuss this with Dr. Athos Gentile, Medical Director and Internist.
“Cholesterol is an indispensable substance for the human body,” explains Dr. Gentile. “It is essential for hormone production, Vitamin D synthesis, and the structural integrity of cell membranes. It is not the ‘enemy’ it is often perceived to be.”
In the bloodstream, cholesterol is transported by lipoproteins. The two primary types are:
-
HDL Cholesterol (High-Density Lipoprotein): Commonly known as “Good Cholesterol.” HDL functions as a scavenger, removing excess cholesterol from the tissues and transporting it back to the liver to be metabolized and eliminated. Maintaining adequate HDL levels provides a cardioprotective effect.
-
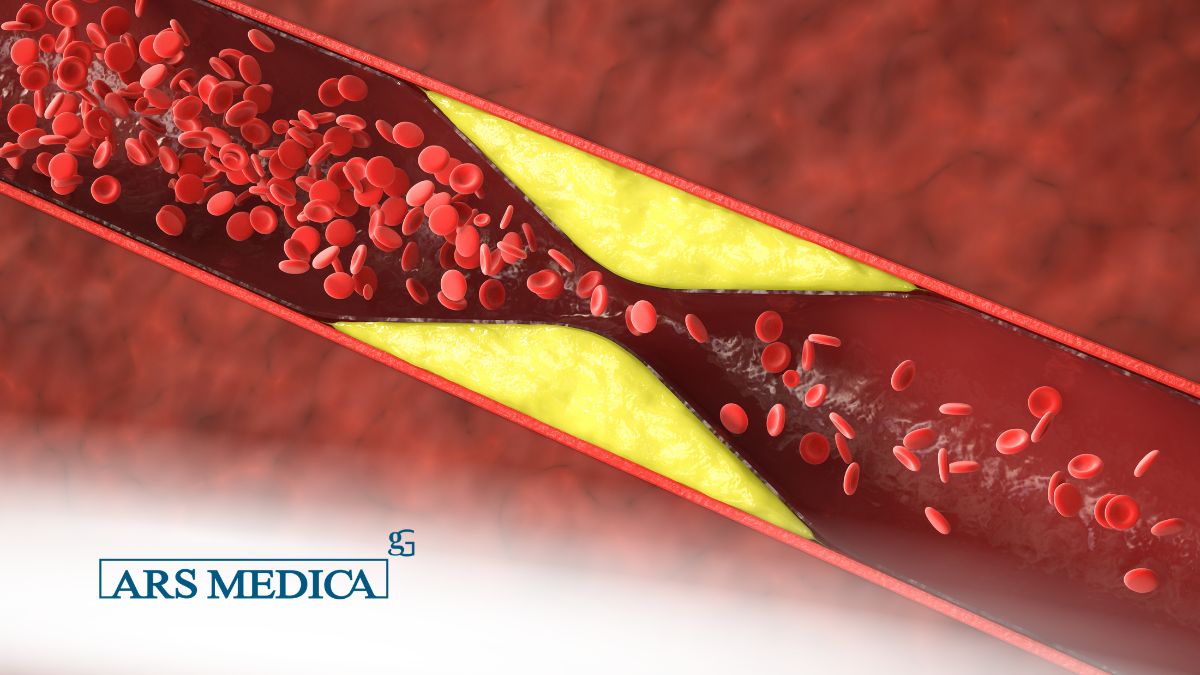
LDL Cholesterol (Low-Density Lipoprotein): Often labeled “Bad Cholesterol.” LDL transports cholesterol from the liver to the peripheral tissues. When present in excess, it can deposit into arterial walls, contributing to the formation of atherosclerotic plaque. Elevated LDL levels are directly associated with increased cardiovascular risk.
Why Total Cholesterol is Not Enough?
A frequent misconception is focusing solely on the total cholesterol count. In reality, cardiovascular risk is determined by a broader clinical picture, including:
-
The Ratio of Total Cholesterol to HDL
-
Triglyceride levels
-
Blood pressure and blood glucose
-
Age, sex, and smoking status
-
Family history of cardiovascular disease
-
Presence of diabetes or metabolic syndrome
Two individuals with the exact same total cholesterol value may have entirely different risk profiles. This is why a specialist’s consultation is indispensable.
The Central Role of the Internist
An Internal Medicine specialist maintains a holistic view of the patient. Rather than reacting to a single out-of-range number, the internist integrates laboratory data with the patient’s clinical history, physical examination, and individual risk factors.
-
Assessing Global Cardiovascular Risk: International guidelines, such as those from the European Society of Cardiology, recommend calculating overall cardiovascular risk before deciding on interventions. Not every elevated LDL requires immediate medication, and not every low HDL indicates disease.
-
Avoiding Redundant Testing: Patients often self-prescribe tests like Carotid Ultrasounds (Doppler), Coronary CT scans, or Stress Tests after seeing an abnormal lab value. Without clinical guidance, these can lead to unnecessary anxiety, over-diagnosis, and avoidable costs.
-
Identifying Secondary Causes: Altered lipid profiles can often be secondary to underlying conditions such as hypothyroidism, insulin resistance, liver disease, or specific medications. Treating the number without addressing the root cause is an incomplete medical intervention.
-
Tailored Therapeutic Strategies: Medication is not always the answer. For many, targeted lifestyle modifications—such as dietary adjustments, physical activity, weight management, and sleep quality—are sufficient to optimize the lipid profile. When therapy is necessary, it must be customized to the individual’s specific risk.
Beyond the Numbers
Blood tests are a diagnostic tool, not a diagnosis in themselves. Cholesterol values must be interpreted within the context of the individual, not in isolation. The internist’s approach ensures that the patient is neither undertreated nor subjected to excessive intervention.
Before starting a treatment or undergoing further scans, always have your lipid profile reviewed by a specialist in internal medicine. True medicine is not the correction of an altered parameter; it is the care of the person as a whole.









